

As QPP MIPS 2020 is approaching the end of the performance year, P3Care has decided to revisit the changes and flexibilities in response to COVID-19. It has been a tough year, especially for our heroes – the healthcare providers. In fact, the pandemic made the healthcare industry work more than its capacity.
Besides relaxation in compliance obligations, the purpose of these flexibilities is to assist physicians in a state of emergency.
COVID, even after the vaccine is out and about, is still pretty much there. The federal agencies alongside CMS work to immunize people in the fifty states. That’s more than enough a country could do but there is still work to be done.
On the whole, the Joe Biden administration seems to care for the environment a lot. We will continue to see improvements in the natural order of things from here on.
Let’s dive into the final rule 2020 and the changes across the MIPS 2020 performance categories.
COVID-19 pandemic has affected every sector of the healthcare industry. There is no surprise there. However, the effects are not similar in every medical practice. Some practices suffered financially, while some came under pressure due to a high surge of patients.
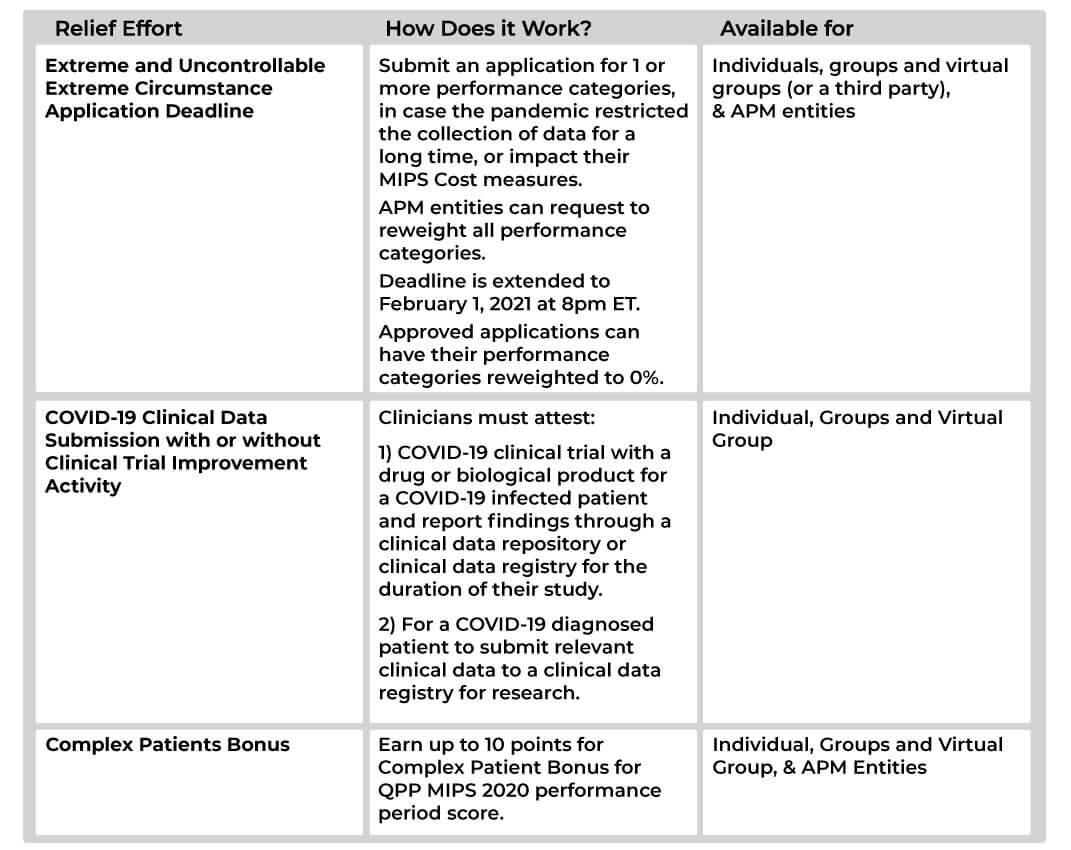
Meanwhile, CMS realized that physicians and MIPS Qualified Registries might not report QPP MIPS 2020 data effortlessly. Therefore, the authority allowed clinicians, groups, and virtual groups to request to reweight one or more performance categories under the Extreme and Uncontrollable Circumstances policy.
As you know, our healthcare facilities are still struggling with the extreme pandemic situation. Therefore, CMS also extended the deadline to apply for Extreme and Uncontrollable Circumstances until February 01, 2021, Monday.
Moreover, CMS introduced a new MIPS Quality measure under Improvement Activities (IA) for the QPP MIPS 2020 reporting. Under this measure, eligible clinicians can receive credit for their quality healthcare services (related to COVID-19) that improve the overall patients’ outcomes.
For the 2021 performance year, QPP (Quality Payment Program) has released the Final Rule:
APM Entities can request for extreme and uncontrollable circumstances exception to reweight QPP MIPS 2020 performance categories
The current Complex Patient Bonus is revised to account for the complex patients’ treatments during the pandemic. Moreover, Clinicians, groups, virtual groups, and APM entities can earn up to 10 bonus points in their QPP MIPS 2020 score.
We think that these steps from the CMS encourage clinicians to participate in the QPP MIPS 2020 despite the corona. It is an effort to facilitate PHE (Patient Health Examination) while considering the difficulties of affected physicians.
If one good thing happened during the pandemic, it is the use of technology at every forum. Obviously, the Healthcare industry is no exception.
Technology has been a savior throughout the pandemic in the form of telehealth. When there was risk catering to elective face-to-face visits, physicians kept in touch with their patients via technology. It helped them to keep the revenue cycle running while restricting the virus exposure.
Not just doctors but MIPS Qualified Registries are also using the latest ways to compile reporting data efficiently to avoid health security threats.
Another update is for ACOs (Accountable Care Organizations) that CMS considers them affected by the extreme condition. Thus, the Shared Savings Program’s extreme and uncontrollable circumstances policy applies to them. Besides, they do not have to file for Consumer Assessment of Healthcare Providers and Systems (CAHPS). In return, ACOS can receive full credit for the high patient experience.
All in all, CMS also supported the expanded use of PHI (Protected Health Information). Thus, we would see more technology-based services such as telephone-based evaluation and management services for CMS Web Interface and the CAHPS. Such services will assist in managing the QPP MIPS survey.

